
Which Business Solutions Can Enhance Your Plan?
With a deep bench of talented actuaries, lawyers, a physician, other professionals, and sophisticated technology, we can tackle even your toughest business problems. We can:
- Select business partners
- Design value-based benefits
- Develop contribution strategies

Do You Have the Right Business Partners?
By using best practices to select the right business partners we can save you money and make it easier to administer your plan. We can help:
- Provide actuarial expertise on the development and pricing of vendors’ products
- Guide you on the value of clinical programs with assistance from our on-staff physician
- Assist with contracts and compliance issues
- Give independent, conflict-free advice because we do not accept commissions or other payments from vendors

How Can Your Plan Benefit from Value-Based Designs?
Value based benefit designs encourage participants to use the most cost-effective services and providers and to take an active role in managing their health. We can:
- Evaluate the impact of changes on the plan and its participants
- Design benefits that encourage better use of the healthcare system
- Implement wellness programs that provide meaningful benefits
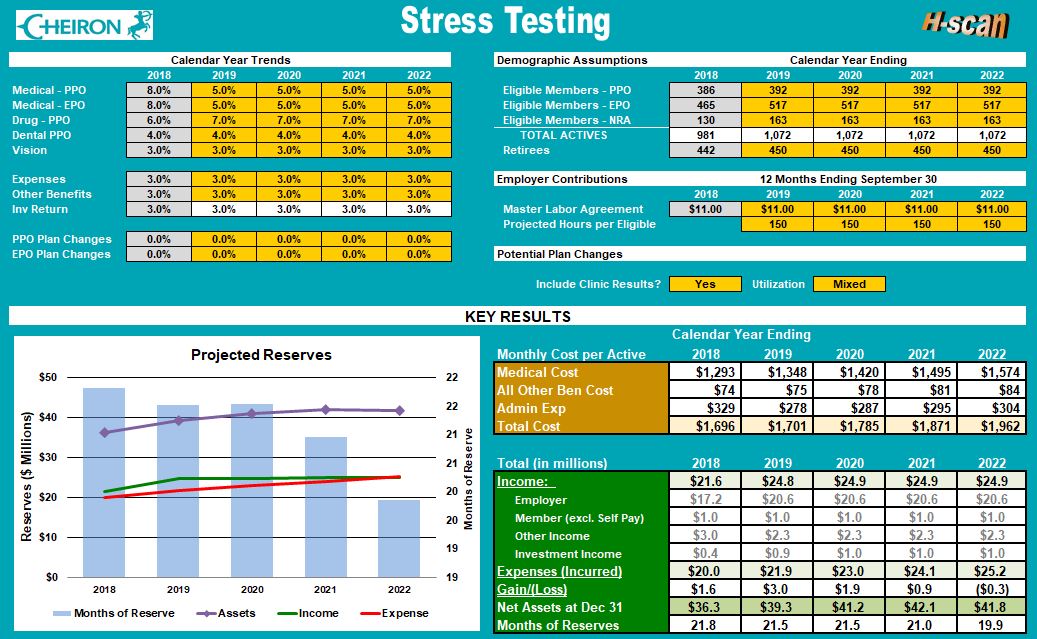
What Is the Best Contribution Strategy for Your Plan?
Plan sponsors often find it difficult to determine how to allocate costs between the plan, participants, and patients. Using the plan’s data, combined with our proprietary databases and expertise, we can:
- Produce accurate financial projections
- Evaluate changes in eligibility, benefit designs, contributions, and long-term funding policies
- Stress-test multiple scenarios using H-Scan, our flagship interactive tool
